Many adults experience back or neck pain at some point in their lives. This discomfort can stem from a specific spinal issue known as a herniated disc. When individuals develop this condition, daily activities frequently become difficult to perform. The resulting physical limitations may disrupt work routines, exercise regimens, and simple household tasks. By learning about the signs of spinal disc issues, patients can make informed decisions regarding their medical care.
What Is a Herniated Disc?
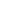
The human spine consists of a series of bones called vertebrae. Between each of these bones rests a specialized structure known as a spinal disc. These discs act as shock absorbers for the body, allowing the spine to flex and bend smoothly. Each one features a firm, rubbery exterior layer that protects a soft, jelly-like center. A herniated disc develops when the tough outer shell sustains damage. The exterior casing can tear or weaken due to the natural aging process, which causes the discs to dry out and break down over time. When a rupture occurs, the soft inner material pushes outward through the compromised outer layer.
What Are the Symptoms?
When the inner material of a spinal disc protrudes, it often presses against nearby spinal nerves. This nerve irritation produces a distinct set of physical signs. Individuals typically feel localized pain in the immediate area of the affected disc, which most commonly occurs in the lower back or the neck.
The discomfort rarely remains confined to a single spot. Nerves travel from the spine to other parts of the body, so the irritation frequently causes radiating symptoms. As a result, patients may experience burning sensations, sharp pain, or tingling that travels down their arms or through their legs. The exact path of the radiating pain depends entirely on which specific spinal nerve is compressed by the bulging disc material.
In situations involving severe nerve compression, patients might experience noticeable muscle weakness. This weakness can manifest in the upper or lower extremities. A person might find it unusually difficult to grasp small objects with their hands or notice a loss of balance and instability while walking.
What Follows a Diagnosis?
Medical professionals utilize several methods to address both disc pain and nerve irritation. A comprehensive care plan targets the root cause of the discomfort, helping restore functionality and improving quality of life. Physical therapy serves as a foundational approach for managing spinal nerve compression. Therapists can use exercises, stretching, and massage to relax tight muscles. These targeted movements relieve the physical pressure on the affected nerve and increase local blood circulation to aid the healing process.
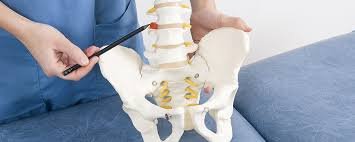
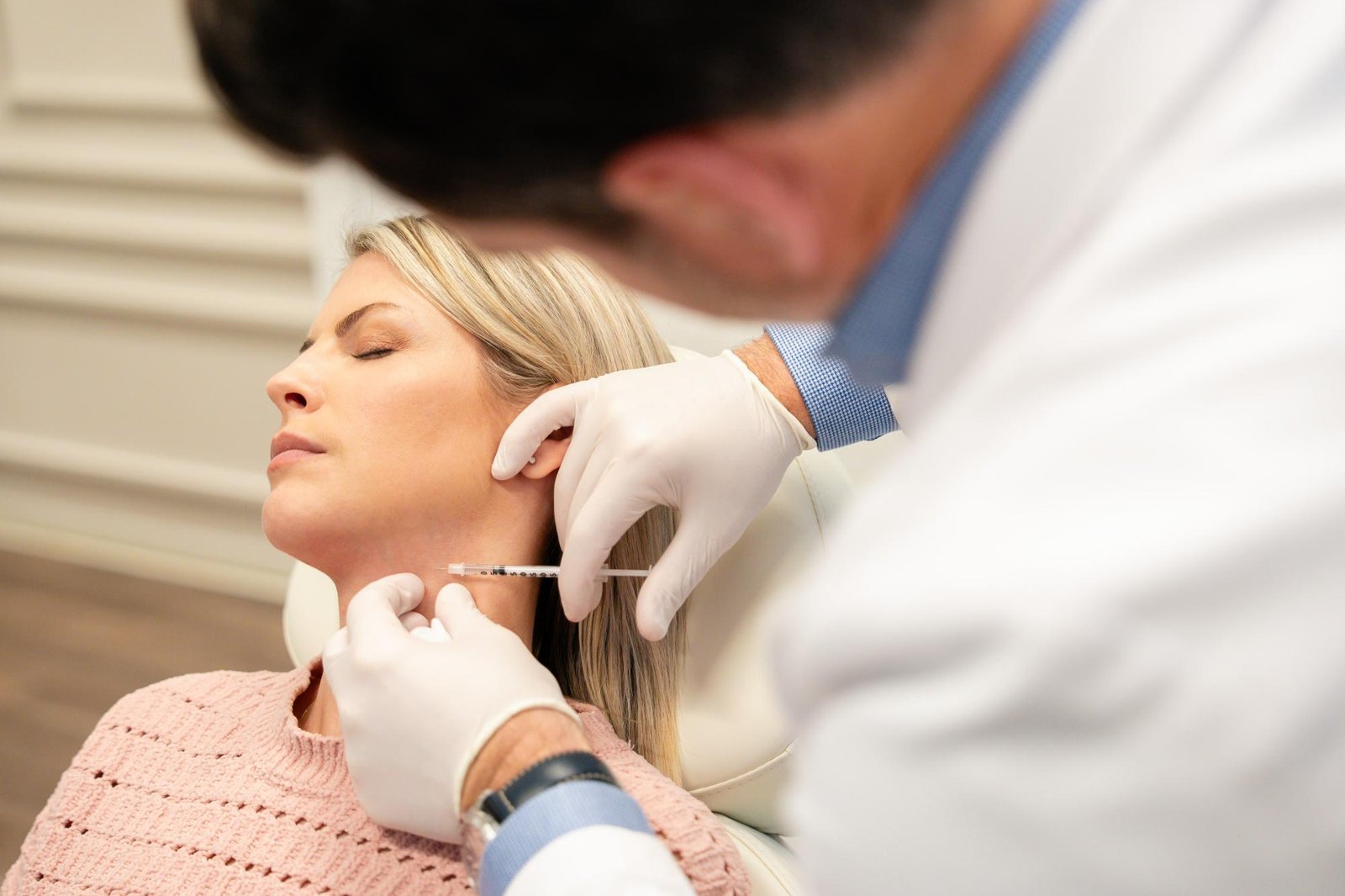
When conservative physical therapies do not provide adequate relief, physicians might utilize epidural steroid injections. Radiofrequency ablation offers another medical option for managing stubborn nerve pain. During this procedure, a specialist uses a highly precise needle that emits radiofrequency energy. This energy creates a tiny wound on the affected nerve, which disrupts the pain signals from reaching the brain. For specific cases, a doctor might perform surgery.
Seek Professional Pain Management Care
While resting for a short period can initially help with back pain, prolonged physical inactivity can lead to complications. Receiving a formal evaluation from a medical specialist gives you a definitive diagnosis and provides a clear understanding of your specific spinal condition. Delaying an evaluation can allow nerve compression to worsen over time. Reaching out to a qualified healthcare provider allows you to address the root cause of your discomfort and take active steps toward regaining your mobility.





Leave a Reply