The human foot relies on a complex structure of bones, ligaments, and tendons to support the body’s weight. The natural arch of the foot is either very low or completely absent for some, a condition commonly known as flat feet. This structural variation can alter the way weight is distributed across the lower limbs during movement. Understanding the mechanics of the foot may help individuals recognize the signs of this condition and allow them to take appropriate steps to maintain joint health.
What Is Flat Feet?
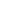
Flat feet develop when the arches on the inside of the feet are flattened, which allows the entire soles to touch the floor when standing. The arch typically creates a visible gap between the inner sole and the ground. Without this gap, the foot lacks its natural shock-absorbing mechanism.
Many individuals with this anatomical feature never experience pain or mobility restrictions. The lack of arch support can lead to distinct physical challenges over time. Pain may develop in the midfoot or ankle region. The condition can also cause the ankles to turn inward, which places abnormal stress on the surrounding joints. This misalignment frequently results in swelling around the ankles, as well as aching in the knees, hips, or lower back. Recognizing these symptoms early allows for prompt and effective intervention.
What Causes Their Development?
The development of flat feet stems from a variety of genetic and environmental factors. Some individuals are born with flat feet, a result of their arches never fully developing during childhood. The condition arises later in life for others due to the gradual wear and tear of aging, which weakens the tendons supporting the arch.
Certain health conditions significantly increase the likelihood of developing flat feet. Arthritis can alter the structure of the foot joints, while diabetes affects nerve function and blood circulation in the lower extremities. Obesity places excess pressure on the feet, leading to the gradual collapse of the arches. Traumatic injuries to the foot or ankle also contribute to the condition.
What Does Management Include?
Addressing flat feet involves a combination of supportive therapies and lifestyle modifications. A thorough evaluation by a foot specialist usually includes an assessment of your gait and involves imaging tests like X-rays or MRI scans to view the bone structure. Based on these findings, specific treatments are recommended to alleviate discomfort and improve mobility.
Physical exercises play a significant role in managing symptoms. Stretching the Achilles tendon and the calf muscles may help relieve tension, aiming to prevent pain. Applying ice packs to the affected area can effectively decrease swelling and soothe sore tissues.
Custom orthotic devices offer structural support for the feet. These specially designed shoe inserts help distribute body weight evenly and correct joint alignment. Managing body weight is also a highly effective strategy to decrease the physical load placed on the lower extremities. If a patient has diabetes, routine clinical evaluations are necessary to monitor foot health and prevent complications. When conservative measures do not relieve severe pain, surgical procedures can restore foot stability and resolve the underlying mechanical issues.
Confer With a Podiatrist
Managing foot health requires ongoing attention and expert guidance. If foot pain begins to interfere with your daily routine, seeking a professional medical evaluation is the right course of action. A podiatrist possesses the specialized knowledge required to diagnose structural foot abnormalities and prescribe tailored treatment plans. Prioritizing expert medical care helps maintain joint mobility and sustains long-term physical well-being.



Leave a Reply