The hip joint serves as a primary weight-bearing structure in the human body and facilitates walking, sitting, and basic movement. When hip pain develops, it often restricts these daily functions, diminishing a person’s overall physical capability. Understanding the origins of this discomfort can be a productive step toward restoring movement.
What Causes Hip Pain?
Weight-bearing joints, like the hip, may sustain significant physical stress over a person’s lifetime, which makes them susceptible to various degenerative conditions and acute injuries. Osteoarthritis frequently develops as people age, resulting from the gradual erosion of the articular cartilage that protects the ends of the bones. As this cartilage wears away, the bones rub together. This generates inflammation and hip pain.
Acute injuries also play a significant role in joint distress. Fractures involve breaks in the bone tissue, while dislocations happen when the joint slips entirely out of its natural socket. Another frequent source of joint distress is bursitis. Bursae are fluid-filled sacs that act as cushions between bones and soft tissues. Repetitive motions or excessive friction can irritate these sacs, causing them to swell and generate localized pain in the hip region.
How Does It Impact Mobility?
The hip’s ball-and-socket mechanism supports the body’s entire upper weight while enabling a wide range of motion in the lower extremities. When inflammation or structural damage compromises this mechanism, the direct result is a noticeable decrease in physical mobility. Patients may experience difficulty performing routine tasks. The localized swelling and stiffness restrict the joint’s natural range of motion. Pain may also disrupt restful sleep, which subsequently decreases overall energy levels during waking hours.
How Is It Treated?
Medical providers evaluate joint complaints through a systematic diagnostic process. An initial assessment involves reviewing the patient’s medical history and discussing specific symptoms. Providers ask when the pain started and identify specific activities that aggravate or alleviate the discomfort. A physical examination allows the medical professional to test the joint’s range of motion and pinpoint specific areas of tenderness. To look inside the joint structure, clinics frequently utilize X-ray technology.
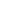
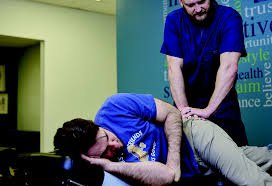
Once a diagnosis is established, providers typically recommend a conservative treatment plan tailored to the specific condition. Minimally invasive approaches may include anti-inflammatory medications to reduce swelling or prescribe custom orthotic footwear inserts to correct gait imbalances. Medical professionals also utilize joint injections to deliver targeted relief. For structural support, providers might suggest the use of walking aids, casting, or bracing. When conservative methods do not yield sufficient improvement, or if the joint has sustained irreparable structural damage, orthopedic specialists may refer the patient to a surgeon for a comprehensive surgical evaluation.
Seek Professional Orthopedic Care
Addressing joint discomfort promptly can prevent localized inflammation from developing into chronic structural damage. Early intervention provides the best opportunity to manage symptoms through conservative, non-surgical methods. By undergoing a formal medical evaluation, patients receive accurate diagnoses and targeted therapies designed to restore physical function. Seeking expert guidance gives individuals the precise tools and knowledge needed to manage joint distress and maintain a functional, active lifestyle.



Leave a Reply