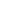
Wound care addresses serious skin injuries, and these may result from pressure or immobility. Pressure ulcers, also called bedsores, need prompt attention because they develop quickly and progress without warning. Proper care helps limit further tissue damage and supports the natural repair process, which takes time and consistent effort. Here is more information on wound care designed for pressure ulcers:
Increasing Protein Intake
Nutrition influences wound healing. Patients may recover more effectively when their diet provides sufficient calories, and medical teams monitor intake to meet the body’s increased demands. Protein is a primary building block of new tissue and aids in repairing injuries. When skin heals, it helps form the structure that closes wounds.
For animal sources, lean meats supply protein, while vegetarians might choose beans, lentils, tofu, or eggs. People may struggle to chew or swallow due to illness; In these cases, liquid supplements offer nutrients in an easier form. Drinking water supports all cellular repair, and monitoring fluid intake is a standard hospital routine.
Reducing Pressure
Pressure is a significant cause of skin breakdown and ulcers. If patients remain in one position, blood flow is blocked at pressure points, and the skin can tear. Caregivers move patients so tissues get regular relief from body weight. Soft cushions and pillows help distribute weight evenly. Special support surfaces like foam mattresses reduce friction on bony areas.
While patients rest, medical workers may turn them regularly to stop pressure. Foam wedges may lift heels, and elbow pads protect delicate skin. Movement, even small adjustments, helps keep blood moving. If a constant force persists, healthy skin tissue is typically damaged.
Doctors use lifts for safe patient transfers, and these help reduce risks. Sliding boards or draw sheets prevent rubbing that leads to skin tears. Wound care teams watch for redness, blisters, or open sores and act quickly if changes appear. Early detection helps to prevent deep tissue injuries, so frequent checks are part of the process.
Changing Wound Dressings
Daily dressing changes help protect an ulcer from further harm, and fresh bandages keep out bacteria. When a dressing becomes wet with fluid or sweat, nurses can switch to a clean covering. Cleanliness is a priority, so supplies are on hand, including:
- Saline cleans the area thoroughly.
- Gauze pads absorb extra fluid to keep skin dry.
- Tape holds the dressing in place around the wound.
These steps help limit risks and help the wound area stay stable until the next change.
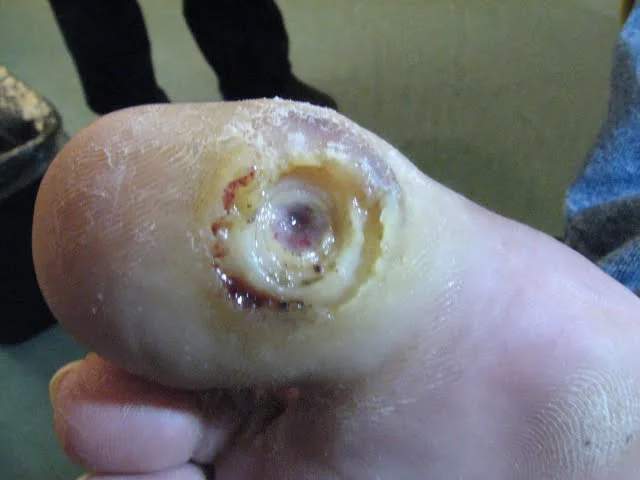
Performing Debridement or Grafts
Deep wounds need extra help to start healing. Surgeons remove dead tissue in a controlled procedure so healthy skin has space to form. This may be uncomfortable, but pain medication blocks these sensations. In some cases, skin grafts cover large areas and support recovery.
Find Wound Care Near You
Pressure ulcers left untreated may result in severe tissue loss or infection. Local clinics and wound care centers provide tests and develop strategies that match your needs. If you notice signs of a pressure ulcer, do not wait to act. Contact your doctor or a wound care nurse today to get an evaluation and start a plan that helps protect your health.



Leave a Reply