Eczema represents a broad medical term for a skin condition that causes the skin to become intensely itchy, red, dry, or distinctly rough. While this specific condition frequently emerges during early childhood, it can develop at any age and present varying degrees of severity. The physical presentation might be long-lasting or flare up sporadically throughout a person’s life. Managing this widespread skin disorder requires a structured approach to daily routine care and targeted medical eczema treatment tailored to each patient.
What Is Eczema?
Eczema functions as a distinct inflammatory skin condition that severely impairs the skin’s natural ability to retain moisture and defend against external irritants. This fundamental barrier dysfunction leaves the outer layers of the skin vulnerable to environmental triggers. Anyone can develop eczema, as it remains a highly common dermatological issue.
Medical professionals identify several key risk factors that increase the likelihood of developing the condition. Individuals with a direct family history of eczema face a significantly higher probability of experiencing symptoms; other predominant risk factors include a personal or familial history of allergies, hay fever, and asthma. Being a child also stands as a primary demographic risk factor. To reduce the likelihood of severe flare-ups, affected individuals can adopt targeted daily habits. Keeping the skin consistently moisturized stands as a primary defense mechanism.
How Is It Detected?
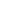
People diagnosed with eczema frequently report severe itching, which prompts an urge to scratch the affected areas. The skin typically presents as excessively dry and notably rough to the touch. Patients regularly observe discolored skin patches, small raised bumps, and areas of cracked or distinctly thickened skin. The affected regions frequently become swollen and highly sensitive to external contact. When left entirely untreated, eczema might lead to secondary skin infections and other disruptive complications.
Medical professionals diagnose eczema primarily through a comprehensive physical examination of the affected skin. A dermatologist closely reviews the patient’s current symptoms and conducts a detailed assessment of their medical history. To reach a precise diagnosis, the provider may complete specialized patch testing or utilize other specific diagnostic tests. These testing methods allow the physician to detect the specific type of eczema or rule out similar-looking skin conditions.
What Does Eczema Treatment Include?
Eczema treatment involves a strict combination of targeted medical therapies and practical home remedies designed to reduce surface inflammation. The most common medical treatments include topical and oral medicines. Applying specific medicated creams to the affected skin helps repair the compromised skin barrier and control persistent itching. In some cases, dermatologists prescribe oral medicines to systematically reduce inflammation.
Light therapy serves as another specialized therapeutic option. Exposing the skin to highly controlled, small amounts of natural sunlight or artificial ultraviolet light can help reduce troublesome eczema symptoms. For localized relief, medical providers might recommend wet dressings. This approach involves wrapping the affected skin in a wet bandage or applying topical corticosteroids directly under the dressing to alleviate severe discomfort.
Meet With a Dermatologist
Securing an accurate diagnosis requires dedicated professional medical guidance. A dermatologist possesses the specialized training necessary to identify eczema, allowing them to construct an effective, individualized care plan. Partnering with a skilled medical provider grants access to an array of treatments designed to improve overall skin health and reduce bothersome complications. Scheduling a formal consultation allows the physician to evaluate your specific symptoms and initiate a structured approach to managing your long-term skin health.




Leave a Reply